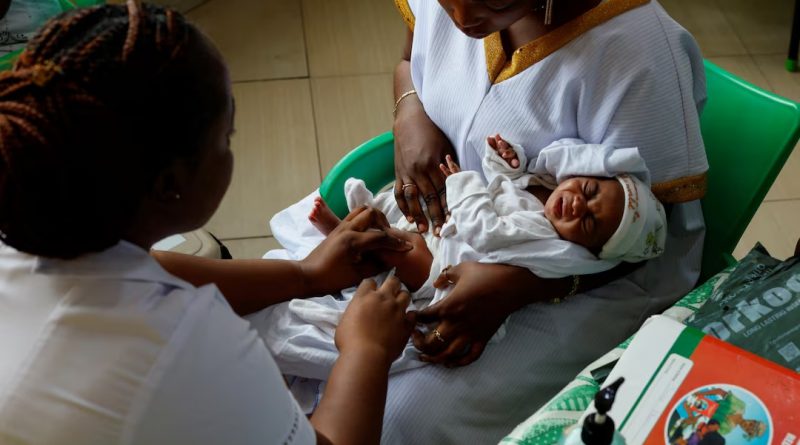
U.S. overhaul of global HIV and malaria supply chain raises fears of treatment disruptions
“There could be immediate risks to service continuity if the transition is rushed or incomplete,”
The United States is restructuring how it delivers life-saving medical supplies for HIV and malaria to low-income countries, a shift that officials and health experts warn could disrupt treatment access across parts of Africa and Asia.
The changes centre on winding down the Global Health Supply Chain Program – Procurement and Supply Management, a U.S.-funded initiative run by Chemonics, which has coordinated the delivery of critical medicines and prevention tools since 2016. According to internal communications and multiple sources familiar with the matter, U.S. officials have been instructed to begin halting implementation of the programme by May 30.
From its inception through 2024, the programme distributed more than $5 billion worth of HIV and malaria-related commodities to 90 countries, with a primary focus on sub-Saharan Africa and parts of Asia. The supplies included antiretroviral drugs, malaria treatments and insecticide-treated bed nets, forming a key component of global disease control efforts.The restructuring follows broader changes to U.S.
foreign aid policy under the administration of Donald Trump, which has prioritised reducing reliance on contractors, cutting budgets and shifting toward direct agreements with recipient governments. The overhaul also comes after the dismantling of the United States Agency for International Development, which had previously overseen much of Washington’s development assistance.
Five sources familiar with the transition said the pace of the changes risks creating supply gaps for essential medicines, particularly in countries with fragile health systems. An internal email reviewed by Reuters warned that accelerating the transition without a clear implementation plan could jeopardise continuity of services.
The communication, sent by the U.S. State Department to staff in 17 African countries and Haiti, directed country teams to prepare for the end of programme operations while outlining potential risks. It did not provide a detailed roadmap for replacement mechanisms, instead asking local offices to identify vulnerabilities and report back to Washington.
A State Department spokesperson said the agency had not issued technical instructions for Chemonics to cease operations by May 30, though the contract is set to expire on September 30 in line with other USAID awards. The official end date is listed as November.
The uncertainty has revived concerns stemming from earlier disruptions. In January last year, a freeze on international aid left millions of dollars’ worth of medical supplies stranded in ports and warehouses worldwide, including HIV drugs and malaria prevention tools. Distribution resumed only after waivers were granted for life-saving interventions.
Six sources said the United States has been in discussions with the Global Fund to Fight AIDS, Tuberculosis and Malaria about potentially using its procurement and distribution systems to replace the existing programme. The Geneva-based institution already manages approximately $2 billion in annual purchases for HIV, tuberculosis and malaria programmes through partnerships with national governments and implementing agencies.
However, two sources said earlier plans had envisaged a transition timeline extending to November 2027, allowing sufficient time for procurement cycles and logistical adjustments. Compressing this timeline into a matter of months could create operational bottlenecks, they said, noting that delivering medical supplies to remote areas can take up to a year from order to distribution.
The Global Fund declined to comment on the discussions. The State Department did not directly confirm the talks but said it would rely on pooled procurement mechanisms to secure supplies at competitive prices from private manufacturers.The policy shift is part of a broader “America First” approach to global health funding, which aims to reduce what officials describe as inefficiencies in the existing system.
A strategy document released in September argued that contractor-led programmes had contributed to waste and inflated costs, and emphasised direct funding for frontline services and national governments.
Under the new approach, Washington has signed 28 bilateral health agreements with partner countries and is increasingly channeling funds directly to national authorities. It also plans to use private logistics firms to handle distribution rather than relying on large development contractors.
Recent agreements with countries such as Kenya, Rwanda and Uganda include commitments to increase domestic health spending alongside U.S. funding. However, implementation has encountered obstacles. In Kenya, a proposed deal faces legal challenges from activists concerned about data privacy, while negotiations with Zambia have been delayed as officials seek to safeguard national interests.
Health experts and aid practitioners say the transition risks compounding existing vulnerabilities in global disease control programmes. Previous disruptions linked to funding changes have already contributed to shortages of malaria treatments for children and gaps in HIV prevention services in several countries.
The State Department defended the overhaul, describing the current system as outdated and inefficient. A spokesperson said the new model would prioritise value for American taxpayers while maintaining support for critical health interventions.
Despite those assurances, several sources involved in programme delivery said the lack of a detailed transition plan remains a central concern. They warned that without clear coordination between donors, governments and implementing partners, the shift could interrupt supply chains that millions depend on for survival.